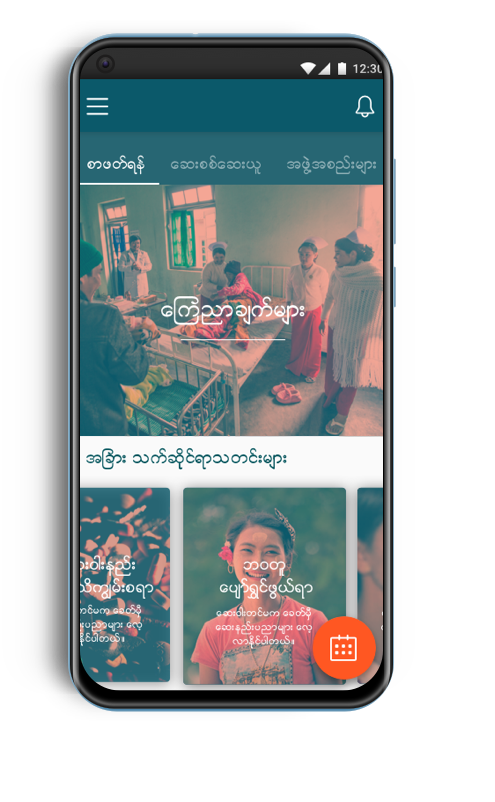
Designing With, Not For
I went to the field. One-on-one interviews, contextual inquiry, and quantitative research across 15 key players in the ecosystem — patients on ART, rural and urban caseworkers, support group leaders, program managers, a country director.
Two personas emerged that shaped every design decision:
Ms. Spotlight — a field representative who is HIV-positive herself. She runs a women’s support group called Lady Queen and shares business opportunities and life advice with members. Her biggest frustration: misinformation spreading unchecked through Facebook, and no reliable way to keep everyone’s details up to date.
Mr. Guidance — a caseworker managing patients spread across multiple towns. Roads between communities can eat an entire day of travel. His contact list was perpetually outdated. Coordinating patient visits and workshop attendance was largely guesswork.
These weren’t edge cases. They were the core users. Designing for them meant designing for the hardest version of the problem.
"Around 240,000 people were living with HIV-AIDS in Myanmar as of 2018. Approximately 70% of the infected people were reported to be receiving antiretroviral treatment (ART) and most of them have achieved viral suppression. Hence, the prevalence of HIV in the general population has been reduced to under 0.6 percent. However, the rate of infection remains high in some groups, such as female sex workers (4.8%), people who inject drugs (13.8%) and men who have sex with men (2.9%). "
UN STUDY OF 2012
The Constraints That Defined the Design
Three things were non-negotiable from the research:
Low digital literacy. Most users had never used an app more complex than Facebook or Viber. Those two platforms became the onboarding strategy — meet people where they already are, use familiar patterns to reduce the learning curve.
Time-sensitive medicine. ART treatment only works if taken consistently, at the right time. A missed dose isn’t just an inconvenience — it has real medical consequences. The app had to make adherence effortless, not just possible.
Patient safety and data trust. This population carries significant stigma. Any design misstep around data visibility or identity exposure could cause real harm. Privacy wasn’t a feature — it was a foundation.